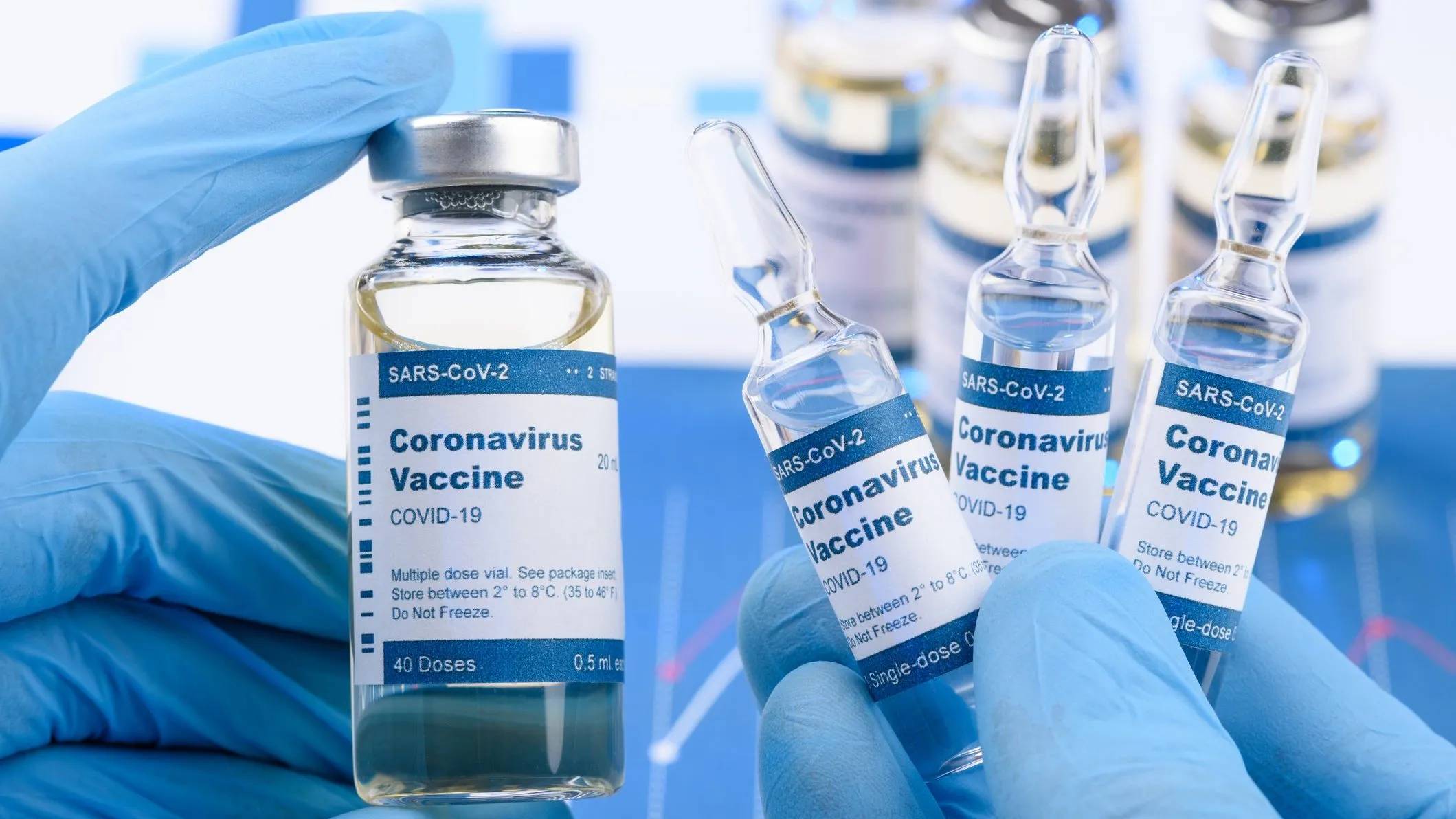
With the coronavirus pandemic at its peak in the United States, the Trump Administration announced, “Operation Warp Speed.” Its goal is to produce 300 million doses of a coronavirus vaccine by January 2021. According to Health and Human Services, Johnson & Johnson, Moderna, and AstraZeneca have already received multi-billion dollar investments in their manufacturing capabilities.
One may begin to wonder, how is the coronavirus vaccine being made? The answer lies behind the science of it all. Viruses are some of the simplest organisms known to man. They lack basic machinery to replicate themselves. For this reason, they use a host, like a human cell. The lack of essential cellular processes makes viruses a poor target for existing therapies like antibiotics. On the other hand, vaccines are simple treatments; they contain pieces of a virus. Delivery of a controlled portion allows the immune system to react. Next, production of memory cells is stimulated. In the event that an individual is reinfected with the same virus, the immune system remembers and responds more effectively than the initial immune response.
The vaccine development process traditionally takes anywhere from 5 to 15 years. The coronavirus vaccine is expected to be approved in 12-18 months. The search starts in a research lab called the preclinical phase. In this phase, researchers test the efficacy of their vaccine on simple animal models or cells. Afterwards, Phase I clinical trials test the vaccine in a small number of healthy people to determine the proper dosage. Phase II tests the treatment in special groups like the elderly to ensure no side effects. Phase III tests tens of thousands of participants. This phase is most likely to provide information about long-term side effects. The final step involves approval of the vaccine. As of September 10, there are 170 vaccine candidates in development worldwide, including 9 candidates in phase III trials.
It’s worth understanding the approaches to develop a vaccine under Operation Warp Speed. For example, Moderna’s vaccine contains Ribonucleic Acid (RNA). RNA can be made into protein, and that’s exactly how the vaccine works. The coronavirus spike protein is synthesized inside the cell. The body can produce antibodies against it to protect from a potential infection. Moderna describes it as the body making its own vaccine.
Another common approach to vaccines is the use of viral vectors; a method being employed by AstraZeneca and Johnson & Johnson. The same way that mosquitoes are vectors which carry viruses between people and animals, viral vectors are designed to carry pieces of other viruses. One such vector is the adenovirus. The adenovirus causes common colds and can be weakened to prevent this. The AstraZeneca and Johnson & Johnson vaccine candidates use adenoviruses. This particular style of vaccine enters the cell and causes an immune response without being lethal like the coronavirus. The immune system will then work to produce antibodies, which is a defense mechanism against pathogens like viruses.
The Knight News sat down with Dr. Dennehy, a professor of Biology at Queens College. Dennehy also doubles as a researcher in the biology department, whose very own lab is studying the coronavirus. According to Dennehy, he anticipates that the vaccine will be widely available in mid-2021.
When asking Dennehy about some of the challenges vaccine researchers face, he explained, “First is safety. It is not simply a matter of dosing patients,” adding, “these patients need to be monitored for some time to ensure that there are no adverse events and that the vaccine is effective in protecting patients. After safety comes logistics and successfully distributing the vaccine to those who need it most.”
Plans are being made to distribute the vaccine to the highest risk people first, including healthcare workers. The real question is, how long will the vaccine provide immunity? There have been two reports of people being reinfected by different coronavirus strains.
Vaccinations offer indirect protection for the immunocompromised. If about 70% of the population has immunity, it is unlikely that an immunocompromised individual will be infected by the virus. Until a vaccine is discovered, the best way to protect yourself and your fellow Americans is to maintain six feet in physical distance from others, wash your hands often, wear a mask, and avoid large gatherings of people.